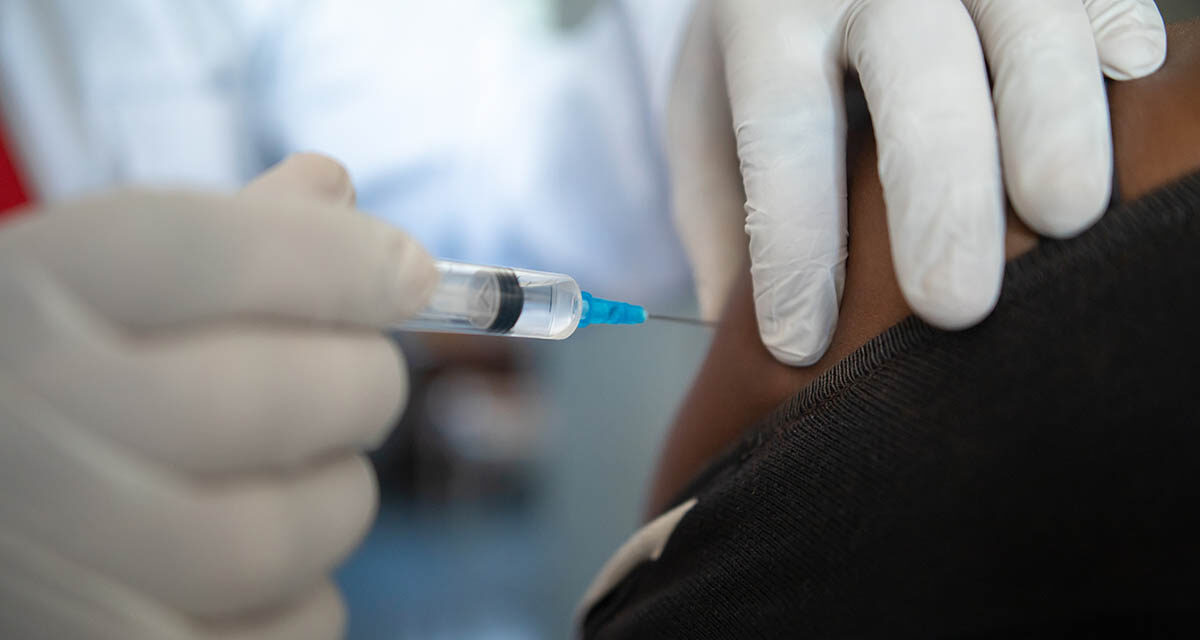
Wits University has begun trials for a potential Covid-19 vaccine this week. Announced at a virtual press conference yesterday, screenings began last week and the first participants will be vaccinated this week in what is Africa’s first Covid-19 vaccine trail
The vaccine project is being led by Wits Professor of Vaccinology Shabir Madhi, who is also the director of the South Africa Medical Research Council (SAMRC) Vaccines and Infectious Diseases Analytics Research Unit (VIDA).
“This is a landmark moment for South Africa and Africa at this stage of the Covid-19 pandemic. As we enter winter in South Africa and pressure increases on public hospitals, now more than ever we need a vaccine to prevent infection by Covid-19,” Madhi said at the conference.
The trials will involve 2,000 volunteers aged 18-65, 50 of whom have HIV. For now the trials are being conducted at multiple sites across Gauteng, but there are plans to extend to other hotspots such as Cape Town in the coming weeks. Half of the participants will be given the potential vaccine while the other half will be administered a placebo. All participants have given written consent to the trial and will take part in it for a full year.
The local clinical trials are part of a collaboration with the University of Oxford and the Oxford Jenner Institute. Before clinical trials can begin in South Africa, they first need to undergo strict regulatory and ethical approval and this trial has been approved by both the South African Health Products Regulatory Authority (SAHPRA) and the Wits Human Research Ethics Committee.
While there have been fears that Africans would be used as guinea pigs for potentially unsafe vaccines developed overseas, this vaccine first began testing in the UK, with 4,000 people already registered for the trials there. Trials are also starting in Brazil and there are plans to start trials on up to 30,000 people in the US soon.
Named ChAdOx1 nCoVr-19, the trial vaccine uses a weakened and non-transmittable version of a virus for the common cold named ChAdOx1. In simplified terms, researchers hope that a similarity between protein spikes in the vaccine and those found on SARS-CoV-2 could allow the body to develop immunity to infection and prevent Covid-19.
The vaccine was made by adding genetic material known as spike glycoprotein to the ChAdOx1 virus. These spikes give the novel coronavirus its distinct spiky appearance and are key to infecting human cells by binding with ACE2 receptors.
“It is essential that vaccine studies are performed in southern hemisphere countries, including in the African region, concurrently with studies in northern hemisphere countries,” said Professor Helen Rees, the chairperson of SAHPRA and Executive Director of the Wits Reproductive Health and HIV Institute (Wits RHI).
“This allows evaluation of the efficacy and safety of candidate vaccines to be assessed in a global context, failing which the introduction of many life-saving vaccines into public immunization programmes for low-middle income countries frequently lags behind those in high-income countries.”
For more details on the science of the vaccine, please visit www.wits.ac.za/covid19vaccine